This article is a revised and updated version of a post originally published in June 2017.
The perceived underfunding of social care was a significant political issue in the 2017 general election. It is easy to forget, however, that the ‘formal’ care sector of nursing and residential homes, plus allied services, is underpinned by a much larger ‘informal’ sector of family and friends of the person being cared for. In a related article, we examined the legislation and policy framework behind this sector. Here, we review the facts and figures relating to informal carers in Northern Ireland. A detailed paper on this topic was recently published by the Research and Information Service (RaISe).

Number of carers in Northern Ireland
Census 2011 defined a carer as a person who provides any unpaid help or support to ‘family members, friends, neighbours or others because of long-term physical or mental health or disability, or problems related to old age’.
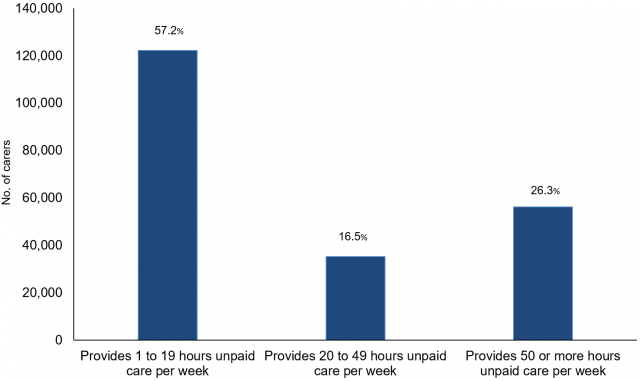
On Census Day 2011, 214,000 people were providing some form of unpaid care, equating to approximately one-in-eight residents in Northern Ireland (12%). This compares with 185,066 in 2001, an increase of 16 per cent. Figure 1 shows that over half of unpaid carers (122,000, 57%) were providing care for between 1–19 hours per week, while 35,000 (17%) were engaged for 20–49 hours per week. Just over a quarter (56,000, 26%) had caring responsibilities for 50 or more hours per week. Using the latest 2017 mid-year population estimates, which show a three per cent increase in population since 2011, there are likely to be around 220,000 people in Northern Ireland with some form of caring role.
Census 2011 data reveals that the majority of carers lie within the 35–64 age band, with one third (33%) aged 35–49, and a further 31 per cent aged 50–64. There are also a significant number of young carers (those aged under 18). For example, 6,700 young people (aged 0–17) in Northern Ireland provide between 1 and 19 hours of unpaid care per week, while a further 960 provide 20–49 hours, and 820 care for 50 hours or more. There are also 11,300 older carers (those aged 75+), more than half (52%) of whom are engaged in caring for 50 hours or more each week. Given the steady rise in population since 2011, these figures are likely to be an under-estimate.
Carers: Who do they care for?
In 2016, data from the Northern Ireland Life and Times Survey (NILT) revealed that a parent or a parent-in-law is the person most likely to be cared for, with more than four out of ten (44%) carers citing this as their main caring role. This was followed by a spouse or partner (29%), other relative (13%) and child (10%). Only 5 per cent cared for a person outside the family.
Carer’s Allowance
Carer’s Allowance (CA) is a non-contributory benefit for people who look after a severely disabled person for at least 35 hours per week. To qualify for the benefit (£64.80), the disabled person must be in receipt of either Personal Independence Payment, Disability Living Allowance or Attendance Allowance.
Table 1, below, shows an upward trend in CA claimants and recipients for the period 2012–2017. At November 2017, there were 46,770 people receiving Carer’s Allowance, a rise of 680 on a year earlier. Of these, 32 per cent were male and 68 per cent female.
| Year | Claimants | Recipients | Credits only |
| 2012 | 62,220 | 38,230 | 23,990 |
| 2013 | 64,600 | 39,910 | 24,690 |
| 2014 | 67,540 | 41,780 | 25,760 |
| 2015 | 70,170 | 43,930 | 26,240 |
| 2016 | 72,630 | 46,090 | 26,540 |
| 2017 | 73,280 | 46,770 | 26,510 |
| Note: Persons in receipt of Credits only refer to those claimants who may be eligible for CA but do not receive it. This is because they receive another benefit which equals or exceeds their weekly rate of CA. Data refers to position at November each year. Source: Department for Communities (2017). |
Issues facing carers in Northern Ireland
Carers UK carries out an annual survey of carers (State of Caring) to build a picture of caring in the four nations of the UK. This section looks at some of the key issues raised by the survey, as well as findings from Census 2011.
Health
Many carers report that caring results in a negative and often lasting impact on their general physical and mental health, but as with the rest of the population, some people with existing disabilities or long-term conditions also take on caring responsibilities. The 2011 Census shows that, in Northern Ireland, over 9,000 carers reported being in bad or very bad health, over half (52%) of whom were providing unpaid care for 50 or more hours per week.
Financial hardship
Taking on a caring role can result in a sharp reduction in household income, especially when the carer is forced to leave work, or reduce their hours to care for someone. The fall in income can be particularly steep if the carer is looking after a partner who has also left work as a result of illness or disability.
While a growing number of people provide unpaid care, a modest increase in Carer’s Allowance (now £64.80) is leaving carers with little scope to manage rising costs.
The State of Caring 2018 survey included over 6,800 respondents throughout the UK, eight per cent of whom came from Northern Ireland. It found that 37% are struggling to make ends meet, while a further 20% said they are in or have been in debt as a result of caring. Little difference in the financial situation of carers was found across the four nations.
Of those who are struggling to make ends meet:
- Nearly two-thirds (61%) cut back on seeing friends and family to cope.
- 80% were cutting back on luxuries.
- Almost three-quarters were reducing spending on hobbies and leisure activities.
- Nearly half (47%) are cutting back on essentials, such as food and heating.
- The 2016 survey found that 1 in 6 (16%) are falling into arrears with housing and utility bills; while others are borrowing money on credit cards (35%); taking out loans (13%); or borrowing from friends or family (30%). Over a third (37%) are using savings to get by, suggesting that their ability to manage is unlikely to be sustainable in the longer term.
Seventy per cent of Northern Ireland respondents to the 2018 survey who are currently providing care said they had suffered mental ill health such as stress or depression as a result of caring, while well over half (56%) said their physical health had worsened as a result of caring.
One respondent stated, “I am worn out physically and mentally drained”, while another said, “I am 79 and wonder how much longer I will have the physical stamina to cope”.
Carers in the 2018 survey were asked about cuts or changes to the care or support services that they, or the person they care for, had experienced in the last 12 months. One in seven carers reported they, or those they support, received less care or support services during the previous year due to a reduction in the amount of support from social services, a service closing without being replaced, or an increase in costs.
One respondent stated (on page 10):
The respite centre is closing in August. There are no other facilities in our area which are suitable so we will lose our respite. This will have a huge impact as I am a single parent and need some time to recharge and relax without having to worry about my sons welfare.
Welfare reform, including changes to disability benefits, may affect eligibility for Carer’s Allowance. For example, should the person being cared for currently claim Disability Living Allowance (DLA), but is deemed ineligible after reassessment for Personal Independence Payment (PIP), then the carer will no longer be eligible for Carer’s Allowance. A new mitigation scheme means that carers who suffer loss will receive a supplementary payment to cover the financial loss for a period of one year.
Caring and work
Census 2011 found that around one-in-seven (119,400, 15%) residents in Northern Ireland aged 16–74 in employment were providing unpaid care. Many working carers find they go months or even years without a proper break.
Across the UK, 2.3 million adults report having given up work to care at some point in their lives and almost 3 million have reduced their working hours. In the 2018 survey, more than a third (38%) of carers reported being in paid employment, almost half (49%) of whom were working full-time. A striking finding was that one-third of those full-time workers were juggling work with providing 50 hours or more of care per week.
Overall, over one third of carers (35%) reported they had given up work to provide care, while a further 16% had reduced their hours in order to support the person they care for. Two in 10 carers (20%) said they had taken a less qualified job, or turned down a promotion, as a result of their caring responsibilities, or that they had retired early in order to provide care.
Young carers
Young carers are an important subset of the carer population, with around 6,500 young people aged under 18 (4% of all carers) engaged in various levels of caring in Northern Ireland. Results from the 2015 Young Life and Times survey indicate that grandparents are the people most frequently cared for (42%), followed by brother or sister (32%), mother (28%), father (10%) and others (10%). Some young people provide care for more than one person. An earlier survey in 2007 found an association between caring responsibilities and income, in that young carers were more likely to come from lower income families.
Summary
The number of carers in Northern Ireland rose by 16 per cent during the decade 2001–2011 to 214,000, and currently stands at around 220,000, or one-in-eight of the population. Around 4 per cent of carers are young people aged under 18. Increased life expectancy and an ageing population mean the demand for carers is projected to increase substantially in coming decades.

